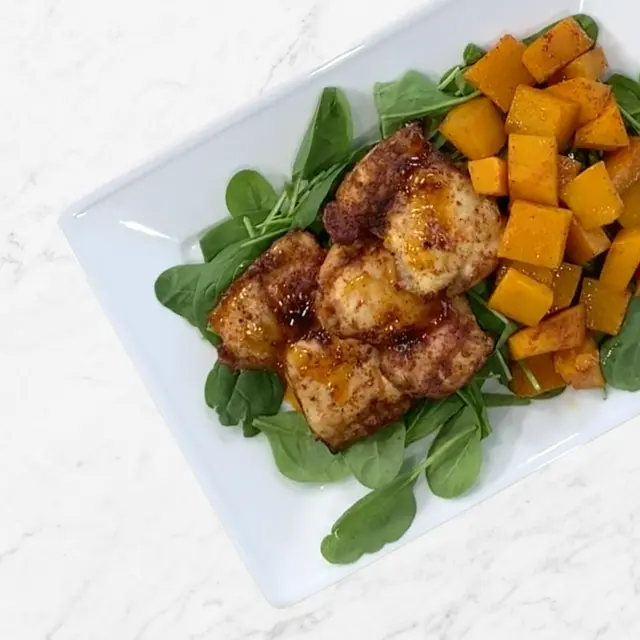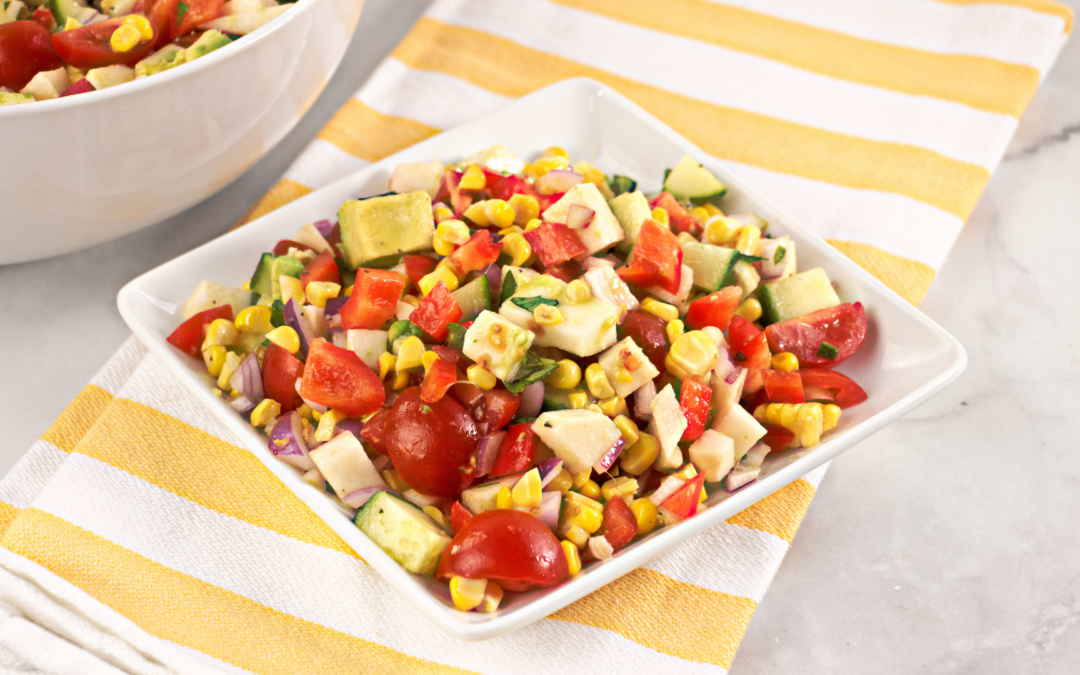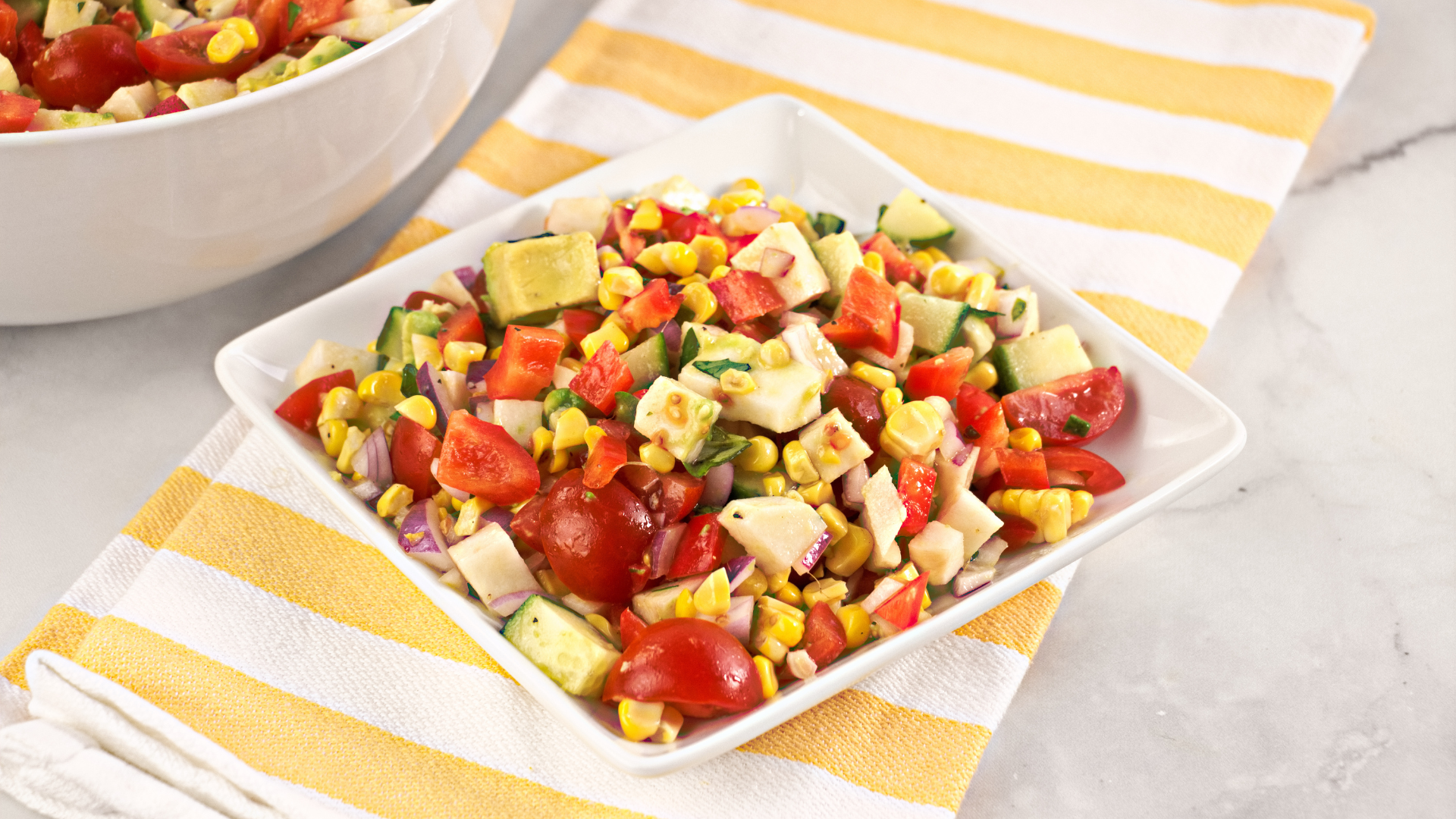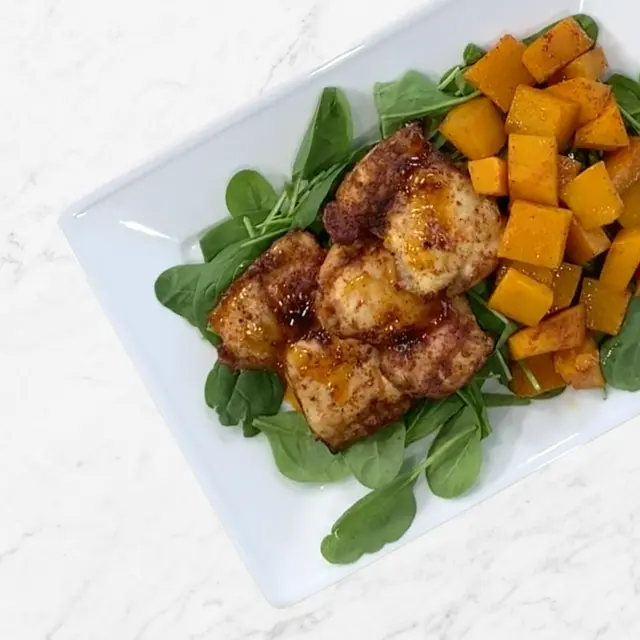
by Kristen Norton | May 14, 2026 | Recipes and Meal Ideas
BBQ Seasoning Mix
- 2 Tbs paprika smoked if desired
- 2 Tbs coconut sugar
- 2 tsp garlic powder
- 2 tsp chili powder
- 1 tsp onion powder
- 1 tsp salt
- 1/8 tsp cayenne pepper optional
Chicken
- 1 Tbs olive oil
- 2 lb chicken thighs boneless and skinless
- 2 Tbs BBQ Seasoning Mix
- salt to taste
- pepper to taste
Make
Add ingredients to glass mason jar fitted with lid – shake to combine and store in a cool, dry place.
Prep
Preheat oven to 375° F. Line baking sheet with parchment paper.
Make
In a glass bowl, toss chicken with olive oil and our BBQ Seasoning mix.
Season with salt and pepper.
Roast until the internal temperature of chicken reaches 165° F, about 20-25 minutes.
Nutrition Facts Calories 297 Total Fat 17g Saturated Fat 4g Cholesterol 180mg Sodium 590mg Total Carbohydrates 2g
Protein 36g Iron 12mg

by Kristen Norton | May 4, 2026 | Well Balanced Wisdom
Whether you go for the atmosphere, to meet up with a friend, or get some work done away from the house, it’s an experience. The smell of coffee, the background noise, the endless menu of options. It feels like a little treat in the middle of your day. And part of the fun is picking out your drink. Espresso, flavored syrups, different milks, foams, whips. The combinations are endless.
You may not realize it, but it’s easy for these coffee concoctions to have similar calories as a meal and exceed your daily added sugar target in just one drink. For example, a grande Starbucks Caramel Ribbon Crunch Frappuccino packs 470 calories and around 60 grams of sugar. For context, the American Heart Association recommends no more than about 25 grams of added sugar per day for women and 36 grams for men. That means one drink can hit double the recommended limit.
The goal here is not to scare you away from a fun coffee order; it’s to bring in some awareness and intentionality. Rather than getting stuck in numbers or feeling like you need to “optimize” every order, it can be helpful to zoom out and check in with what you actually need in that moment.
Order like a Well Balanced Dietitian…
Before ordering, run through a quick mental check-in.
Do I want energy, comfort, or a mix of both? If it’s energy, leaning on a drink with caffeine and some protein can help you feel steadier, while a comfort-driven choice might be more about taste and satisfaction.
Will this keep me going or set me up for a crash? Drinks higher in added sugar and lower in protein or fat tend to digest quickly, which may lead to a quick spike and then drop in blood sugar, while a more balanced option can help sustain energy longer.
And am I having food with this, or is this a standalone drink? A drink on its own may need a little more staying power, like milk or a side with protein or fiber, while a drink paired with food gives you more flexibility to choose what sounds good.
Go-To Balanced Coffee Orders
Take a drink you love and think small, realistic tweaks instead of a total overhaul. These small adjustments can make a big difference without taking away the enjoyment.
- Add protein to your drink by choosing dairy, soy milk, or protein milk if it’s an option. You could also pair your drink with a protein-rich food if you cannot tolerate dairy or soy.
- Keep flavor but dial it back by asking for it “half sweet,” aka one or two pumps instead of four or five. Alternatively, choose a sugar-free option.
- Use cinnamon, cocoa, or vanilla for extra taste without relying only on sugar.
- Choose a smaller size.
Examples:
1. Iced Caramel Latte
Grande, standard version with whole milk: ~250-300 calories, 10g protein, ~32g added sugar, ~12g fat
Well Balanced tweak: (half sweet Grande Iced Caramel Protein Latte) ~230 calories, 29g protein, ~18g added sugar, ~4g fat
A small change in syrup and adding the protein milk cut the sugar nearly in half while bumping up protein substantially, yet keeping the flavor, which means you get sustained energy and comfort. You could also opt for the sugar-free caramel syrup, which would reduce the calories to 190 and the sugar to 8g.
2. Blended Mocha Style Coffee Drink
Standard grande version made with whole milk and topped with cookie crumbles, mocha drizzle, and whipped cream: ~500 calories, 7g protein, ~60g added sugar, ~20g fat
Well Balanced tweak (smaller size, protein milk or 2% milk, half sweet, light or no whip, and no toppings): ~200 calories, 2-9g protein, ~32g added sugar, ~2-6g fat
Even with tweaks, these drinks are often more dessert than coffee. Most of the shift comes from reducing syrup, chocolate sauce, and portion size.
3. Toasted Coconut Latte with Oatmilk
Standard version: ~250-300 calories, 4g protein, ~45g added sugar, ~10g fat
Well Balanced tweak (1–2 pumps of syrup instead of the standard amount, soy or 2% milk): ~200 calories, 11g protein, ~22g added sugar, ~7g fat
The biggest lever here is dialing back added syrup while keeping some sweetness. If you like sweeter, consider adding a stevia or Splenda packet based on your preference. Oat milk contains very little protein, so consider switching to soy, 2%, or adding a balanced food item for steady energy.
Great options that do not need any tweaking or maybe just some:
Cafe Misto ~ 50 calories, 3g protein, 5g added sugar
Half Sweet Honey Almondmilk Flat White ~130 calories, 3g protein, 15g added sugar, 5g fat
Brown Sugar Oatmilk Cortado ~145 calories, 2g protein, 18g added sugar, 4g fat
When You Do Want the Fun Drink
Sometimes you just want the full fun drink experience, and that’s okay. You don’t have to optimize every drink. Especially if it’s an occasional thing! Order it, enjoy it, and try not to rush it. Drinking it slowly can make it more satisfying than rushing through it.
Food For Thought
You don’t have to choose between enjoying your coffee shop drink and feeling good afterward. With a little awareness, you can have both while you relish the coffee shop vibes, good company, and/or a productive work session. Find what works for you and order to support your energy, hunger, and overall well-being.

by Kristen Norton | May 4, 2026 | Nutrition Questions Answered
Most people have feelings about coffee.
Some people can’t live without it and go to bed at night looking forward to their morning cup. While others just don’t feel the same love for it.
Does it spike cortisol? Is it good or bad for my gut health? And what about caffeine jitters?
We can’t talk about coffee without talking about caffeine, and even if coffee isn’t your thing, caffeine often still finds its way in through energy drinks, soda, or other sources. raising the same question: “Is this good for me?” As with everything, it’s truly personal, so we’re sharing insights on both coffee and caffeine to help you make an informed decision.
Why caffeine makes us feel like we can take on the world (or at least those boring, monotonous tasks that need to get done)…
The science-y answer is that caffeine blocks adenosine, a chemical in your brain that makes you feel sleepy. When that signal is muted, you feel more alert, less fatigued, and a little more ready to tackle your day.
It can also sharpen focus, improve reaction time, and even enhance how well certain pain medications work. So yes, caffeine can absolutely help you “do the things.”
Ok, so caffeine helps me do the things… but is it good for my health?
Like most things, it’s nuanced. When we look at the research, the effects of caffeine really come down to how much and how often. Moderate intake—about 3 to 5 cups of coffee per day, or up to 400 mg of caffeine—is consistently linked with a range of fabulous health benefits:
- Lower risk of heart disease, stroke, and cardiovascular-related death
- Reduced risk of type 2 diabetes
- Protection against liver disease, including cirrhosis and liver cancer
- Lower risk of certain cancers, including endometrial cancer
- A strong association with reduced risk of Parkinson’s disease
- Lower rates of depression and suicide
- Overall, a longer lifespan
Does that mean more is better?
No. Once intake creeps above about 400 mg per day, the benefits tend to level off—and for many people, side effects start to show up:
- Anxiety, restlessness, or feeling “on edge.”
- Trouble sleeping
- Racing thoughts or feeling unable to slow down
- Increased heart rate or palpitations
- More frequent urination
Large amounts in a short period of time (think energy drinks or multiple strong coffees close together) can also put extra strain on the cardiovascular system, especially in people who are more sensitive or not habitual caffeine drinkers.
Habitual vs Infrequent Coffee Drinkers
People who don’t usually drink coffee may notice short-term effects like a temporary rise in blood pressure or changes in blood sugar regulation. With consistent intake, these responses tend to lessen over time. Research suggests this is partly because the body adapts to caffeine’s effects on the nervous system, including how it influences signals that regulate alertness and cardiovascular response. Even the familiar caffeine “boost” may feel less noticeable over time.
Coffee is more than just caffeine
Coffee isn’t just a caffeine delivery system. It also contains a range of bioactive compounds, including polyphenols, antioxidants, and other plant compounds that may contribute to health.
Research suggests these compounds may:
- Support blood sugar regulation and metabolic health (though effects vary by individual and context)
- Help reduce oxidative stress in the body
- Be associated with improved liver health and lower risk of fatty liver disease
- Support a more favorable gut microbiome environment
Many of these benefits are observed with decaffeinated coffee, suggesting that compounds beyond caffeine play an important role.
What you put in your coffee matters
Though we see health benefits from moderate coffee consumption, we can’t ignore the coffee additions that can diminish these benefits.
Small additions like a splash of half and half or a modest amount of milk tend to have minimal impact on blood sugar, but larger amounts of sugar, flavored syrups, and sweetened creamers can quickly turn a simple cup of coffee into something that behaves more like a sugar-sweetened beverage in the body. Research consistently shows that added sugars increase blood glucose and insulin demand, and over time, can weaken many of the protective associations seen with coffee alone.
The takeaway is not that you need to drink coffee black, but rather that there is a meaningful difference between a lightly personalized cup of coffee and one that is essentially a dessert in a mug. Choosing simple, less processed additions more often helps preserve the natural benefits coffee can offer while still keeping your routine enjoyable and realistic.
Why caffeine affects everyone differently
Your response to caffeine can vary based on genetics, metabolism, medications, and even lifestyle factors like smoking.
Caffeine is mainly broken down in the liver by an enzyme called CYP1A2. How active that enzyme is in your body determines how quickly caffeine is cleared—and that can vary quite a bit from person to person.
Here are a few situations where caffeine tends to stick around longer:
Pregnancy
During pregnancy, caffeine metabolism slows significantly—especially in the second and third trimesters. This means caffeine stays in your bloodstream much longer than usual. Since it also crosses the placenta and the baby has a very limited ability to break it down, higher circulating levels can build up. That’s why recommendations are more conservative (generally ≤200 mg per day).
Birth control (oral contraceptives)
Estrogen-containing birth control can slow down the activity of the CYP1A2 enzyme. Practically speaking, this means caffeine lasts longer in your system, and you may feel its effects more strongly—or for a longer period of time—compared to when you’re not on it.
Quitting smoking
Smoking actually speeds up caffeine metabolism by increasing CYP1A2 activity. So when someone quits smoking, their caffeine clearance slows back down to baseline. If caffeine intake stays the same, it can suddenly feel like “too much”—leading to jitteriness, anxiety, or trouble sleeping. This is an often-overlooked adjustment during that transition.
Genetics (slow vs. fast metabolizers)
Some people naturally have a slower version of the CYP1A2 enzyme due to genetic variation. These “slow metabolizers” break down caffeine more gradually, meaning it stays active in the body longer. Research suggests they may be more sensitive to the negative effects of higher caffeine intake, particularly when it comes to blood pressure and cardiovascular risk.
On the flip side, “fast metabolizers” clear caffeine more quickly and may tolerate moderate intake with fewer noticeable side effects.
Coffee and sleep
Because how long caffeine stays active in your body varies from person to person, not surprisingly, caffeine doesn’t affect everyone’s sleep in the same way.
Especially if you are a slow caffeine metabolizer, caffeine can still be active in your system hours later and may subtly affect sleep quality, including how easily you fall asleep and how restorative your sleep feels.
If sleep has been a concern, one of the simplest strategies to experiment with is adjusting the timing of your last caffeine intake to earlier in the day.
Coffee and gut health
Coffee can play a supportive role in gut health. Both regular and decaf coffee contain polyphenols that act as fuel for beneficial gut bacteria, helping increase microbial diversity and the production of short-chain fatty acids linked to metabolic and immune health.
At the same time, coffee stimulates the digestive tract. It increases gastric acid production and promotes movement in the intestines, which is why many people notice a bowel movement shortly after drinking it. For individuals with GERD, this increase in acid can worsen reflux symptoms, and for those with IBS-D, the stimulation of gut motility can lead to urgency or looser stools.
While coffee can support gut health at a microbiome level, symptom response matters. If you have a sensitive digestive system, experimenting with timing, amount, or even switching to decaf may help you find a balance that supports both your gut bacteria and your day-to-day comfort.
Coffee and cortisol
Caffeine can cause a short-term increase in cortisol, a hormone involved in alertness and energy regulation. There is a popular claim that coffee on an empty stomach or it too soon after waking meaningfully disrupts cortisol rhythms. Current evidence does not support this for healthy individuals.
Cortisol naturally peaks in the morning as part of your circadian rhythm, whether you drink coffee or not. Adding caffeine during this window may slightly increase that rise, but studies show the body adapts in regular coffee drinkers, and these changes are not considered clinically significant in healthy adults.
Where it does get more individual is how you feel. If you are already waking up feeling wired, anxious, or stressed, caffeine can layer on top of that and amplify those sensations. In that case, it may be worth experimenting with delaying or reducing your first cup. But if you wake up feeling steady and energized, there is no strong evidence that you need to avoid coffee in the morning or wait a specific amount of time.
Bottom line: coffee does have a mild, short-term effect on cortisol, but for most people, it is not harmful. Pay attention to your own stress and energy levels. If you are already feeling on edge in the morning, reconsider that cup of coffee. Otherwise, enjoy it without overthinking the exact timing.
Coffee and Cholesterol
Coffee contains a compound called cafestol, which has been shown to increase serum cholesterol levels. The concentration of cafestol varies dramatically depending on how the coffee is prepared:
High Levels: Cafestol is highly concentrated in unfiltered coffee, such as French press, Turkish, or Scandinavian boiled coffee.
Intermediate Levels: It is found in moderate amounts in espresso and coffee made in a Moka pot. *While espresso contains intermediate levels of cafestol, moderate consumption of espresso-based coffee may not have the same dramatic effect on serum cholesterol levels as boiled, unfiltered versions.
Negligible Levels: Cafestol is virtually absent in drip-filtered, instant, and percolator coffee because the paper filters trap the compound.
Research has shown that high consumption of unfiltered coffee (averaging 6 cups per day) can increase low-density lipoprotein (LDL) cholesterol by 17.8 mg/dL.
In summary, if you are concerned about cholesterol, filtered or instant coffee is the safest choice, as they contain negligible amounts of the cholesterol-raising compound cafestol
So… should you drink coffee?
For many people, coffee can absolutely be part of a healthy lifestyle and offer some meaningful health benefits. But more isn’t always better, and how you feel matters just as much as what the research says.
A few simple things to consider:
- How do you feel after you drink it?
- Do you need a lot of added sugar and sweeteners to enjoy your coffee?
- What’s your quality of sleep when you drink coffee in the afternoon?
- Are you relying on it to push through exhaustion?
- Does it support your routine or work against it?

by Kristen Norton | Apr 28, 2026 | Recipes and Meal Ideas
- Plantains
- 2 plantains sliced
- 3 Tbs olive oil
- salt to taste
- Mojo Verde
- 1/2 jalapeño pepper chopped
- 4 cloves garlic roughly chopped
- 1 cup cilantro roughly chopped
- 1 Tbs vinegar white
- 1/2 cup olive oil
Prep
Preheat oven to 450°F.
Peel plantain and slice a quarter-inch thick diagonally.
Make
Toss plantain slices gently in oil and salt to taste. Place flat on a sheet pan lined with parchment paper.
Bake for 10 minutes then flip and smash the plantain until flat. You can use the bottom of a clean jar to do this.
Bake for another 10 minutes until browned.
Prep
Roughly chop jalapeño, garlic, and cilantro. To control spice level, you can avoid membrane and seeds of jalapeño for a milder heat.
Make
Add all ingredients to a food processor and blend till smooth.
Nutrition Facts: Calories 499 Total Fat 38g Saturated Fat 5g Sodium 9mg Total Carbohydrates 44g Dietary Fiber 3g Total Sugars 24g Protein 2g Calcium 13mg Iron 1mg Potassium 695mg
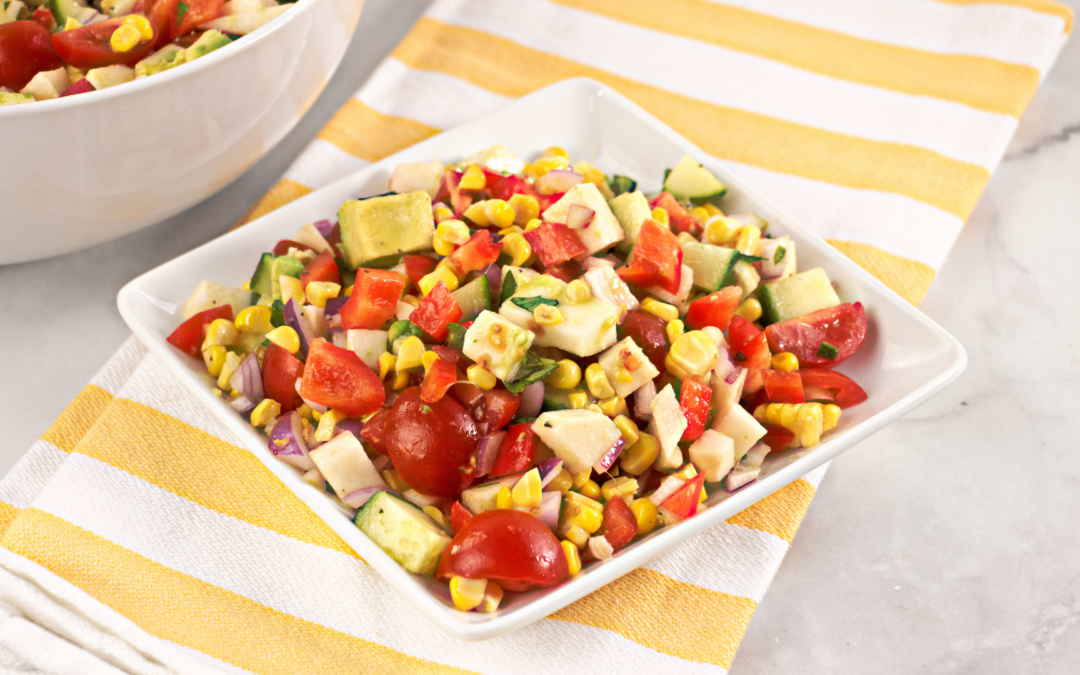
by Kristen Norton | Apr 21, 2026 | Recipes and Meal Ideas
- 4 ears corn shucked
- 1 bell pepper red, chopped
- 1 English cucumber chopped
- 1 jicama small, peeled and cubed
- 1 avocado cubed
- 1/2 onion red, chopped
- 1 pnt cherry tomatoes quartered
- 1/2 cup basil leaves chopped
- 1/3 cup olive oil
- 3 Tbs apple cider vinegar
Prep
Preheat grill to medium-high. Grease the grates.
Prepare all vegetables according to prep instructions.
Make
Brush corn with some of the olive oil while it is grilling, rotating to slightly char all sides.
Remove corn from the grill to cool. Place cob in a deep bowl and remove kernels while holding cob upright. You can also hold corn upright in a bundt pan to capture kernels as you slice them off from the cob with a paring knife.
Add prepped vegetables and corn to a large bowl and toss with remaining olive oil and vinegar.
Season with salt and pepper to taste.
Nutrition Facts: Calories 291 Total Fat 16g Saturated Fat 2g Sodium 16mg Total Carbohydrates 36g Dietary Fiber 11g
Total Sugars 8g Protein 5g Calcium 36mg Iron 202mg Potassium 769mg

by Kristen Norton | Apr 7, 2026 | Recipes and Meal Ideas
- 3 pounds pork loin
- 3 cloves garlic minced
- 1 tbsp rosemary fresh, chopped
- 4 tbsp Dijon mustard
- 2 tbsp maple syrup
- 2 tbsp thyme dried
- 2 tbsp oregano dried
- salt to taste
Prep
Preheat oven to 350° F and line a baking dish with parchment paper.
Pat pork loin dry.
Mince garlic and chop rosemary.
Make
In a small bowl, whisk together mustard, maple syrup, garlic, and herbs.
Season with salt to taste.
Brush paste over the surface of the pork loin.
Roast uncovered for about 45 minutes or until internal temperature reads 145° F.
Remove the roast from the oven and let it sit for about 10 minutes.
Slice into medallions and serve with any remaining juices in the pan.
Nutrition Facts: Calories 466 Total Fat 20g Saturated Fat 6g Cholesterol 181mg Sodium 376mg
Total Carbohydrates 7g Dietary Fiber 1g Total Sugars 4g Protein 61g Calcium 59mgIron 2mg Potassium 852mg

by Kristen Norton | Mar 31, 2026 | Well Balanced Wisdom
Dairy gets a lot of attention in health circles. Some say it’s inflammatory, others say it’s perfectly fine. So what’s the deal? At Well Balanced Nutrition, we consider the evidence and take a personalized approach: there’s no one-size-fits-all answer.
Is Dairy Inflammatory? What Research Shows
Research doesn’t support the idea that dairy is pro-inflammatory for most people. In fact, observational studies link regular dairy consumption to lower rates of type 2 diabetes, cardiovascular disease, and other chronic conditions when part of an overall healthy dietary pattern. More robust studies that combine results from many clinical trials have found that consuming dairy can lower signs of inflammation in the body and may also increase helpful compounds that protect against inflammation. That said, individual responses can vary, and factors like the type of dairy and a person’s overall health play a role.
Not All Dairy Is the Same
Dairy is a diverse food group that includes a wide range of options, each with its own unique characteristics. Take cheese, for example, there are countless varieties, each differing in nutrient profile and makeup. Milk also comes in several forms, from fat-free and low-fat to whole. Different dairy foods can affect the body in different ways, partly due to differences in fermentation and how they interact with the gut.
Some studies show that fermented dairy, like yogurt and kefir, may help lower inflammation and support gut health. Hard cheeses and cultured dairy products are also often easier to digest than milk for people with lactose intolerance.
When Dairy Can Cause Digestive Issues
For some people, dairy can trigger uncomfortable digestive symptoms. Those with lactose intolerance or other gut sensitivities may benefit from a temporary elimination of dairy, followed by a reintroduction to identify if, how much and what types of dairy are a concern. If symptoms improve without dairy and then recur when it’s reintroduced, that’s a strong sign of intolerance.
Managing lactose intolerance is highly individualized, but most people can still enjoy dairy without digestive distress. Research shows that many individuals tolerate small amounts of lactose, especially when consumed with meals, so having smaller portions can help reduce symptoms. Choosing lower-lactose options like aged cheeses and yogurt (which contains live cultures that help break down lactose) is often well tolerated. Lactose-free milk and dairy products provide yet another option. For some, using lactase enzyme supplements before eating dairy can be effective.
The Bottom Line on Dairy and Your Health
Dairy doesn’t need to be feared or eliminated by default. Overall, studies tell us that dairy either has a neutral or anti-inflammatory benefit. The most important factor is personalization: noticing how your body responds, choosing types you tolerate, and including them as part of a nutrient-rich, balanced diet. For many, dairy can be a healthy component of everyday eating and a good source of protein and micronutrients. At Well Balanced Nutrition, we help clients figure out the right approach for their unique bodies. Your gut, your tolerance, your plan. Reach out today to book an appointment.

by Kristen Norton | Mar 31, 2026 | Well Balanced Wisdom
Have you been told to follow an anti-inflammatory diet to improve your health, and wondered about two things?
- Can a healthy diet really reduce inflammation?
- How do I follow an anti-inflammatory diet?
The answer to the first one is yes! Available evidence tells us that a healthy diet can meaningfully reduce chronic inflammation, especially when it follows a Mediterranean‑style, plant‑forward pattern. We’ll break down what that means with 3 simple ways to start an anti-inflammatory diet, but let’s briefly define inflammation first.
What Is Inflammation (And When Is It a Problem?)
Inflammation is your body’s natural defense system, and understanding it is the first step in learning how to reduce inflammation with diet. It helps fight infections, heal injuries, and keep you healthy.
Inflammation becomes a hidden threat when it sticks around long after it’s needed. This is referred to as chronic low‑grade inflammation, and it can be quietly damaging tissues and disrupting normal body functions over months or even years.
Chronic inflammation is a driving force behind disease development and progression. It’s linked to conditions like heart disease and diabetes to cancer, dementia, and autoimmune conditions. It also accelerates aging, contributing to frailty, bone loss, muscle decline, and overall decline in organ function.
The encouraging news is that diet and lifestyle play a powerful role in inflammation—and they’re factors you can control.
How Diet and Lifestyle Affect Inflammation
Chronic inflammation can be influenced by several lifestyle factors, including:
- Nutrient-poor diet high in ultra-processed foods
- Chronic stress
- Poor sleep
- Lack of physical activity
- Smoking or excessive alcohol intake
While all of these factors matter, we’ll focus on practical, consistent actions you can take to improve your nutrition. You don’t need a complete overhaul—just a few intentional shifts can make a meaningful difference over time. Here are three evidence-based ways to help decrease inflammation with food.
Three Simple Ways to Start an Anti-Inflammatory Diet
1. Eat More Antioxidant-Rich Foods
Antioxidants help calm inflammation in two ways. First, they neutralize harmful molecules called free radicals. When too many of these accumulate, they can damage cells and trigger inflammation.
Second, they flip off the switches that tell the body to stay inflamed, while turning on the switches that protect our cells and keep them healthy.
Plant foods rich in antioxidants
- Berries
- Citrus fruits
- Leafy greens
- Sweet potatoes
- Tomatoes
- Bell peppers
- Broccoli and Brussels sprouts
- Nuts and seeds
- Turmeric, cinnamon, oregano, thyme, cloves
- Green tea, black tea, coffee, cocoa, hibiscus tea
Antioxidants come in many forms, and each type protects your body in a slightly different way. A combination of antioxidants from a variety of plant foods is more effective than a large amount of just one type.
Nutrition Challenge: Boost your body’s defenses by including multiple plants at each meal.
Recipes like this antioxidant-rich smoothie can make it easier to add plant foods to your routine:
→ Healthy Chocolate Fudge Smoothie
2. Eat Foods High in Omega-3 Fatty Acids
Higher omega‑3 intake has been linked to lower inflammation in the body. Omega-3 fats work in a few ways: they help your body make compounds that calm inflammation instead of fueling it, and they also support molecules that actively help your body resolve inflammation and repair tissues. Essentially, eating more omega‑3s shifts your body’s chemistry toward a calmer, healthier state.
Marine sources:
- Salmon
- Sardines
- Mackerel
- Trout
A simple way to include these nutrients is a quick salmon dinner like this one:
→ Avocado Lime Salmon
Daily Goal:
- 250–500 mg of EPA + DHA for general health (about 1–2 servings of oily fish per week or a standard supplement)
- 1.5–2 g if aiming to reduce inflammation (3.5–5 ounces of oily fish daily or a mix of fish and supplements)
- Keep supplementation under 3 g unless advised by a professional
Mercury Tip: Choose low-mercury fish like salmon, sardines, trout, or anchovies. Brands like Safe Catch test for mercury so you can eat fish safely every day.
3. Eat To Support a Healthy Gut
A healthy, balanced gut microbiome can send anti-inflammatory signals to your body. One of the most effective ways to support a healthy gut is by eating a variety of fruits, vegetables, whole grains, and legumes. The fiber in these foods acts as a prebiotic, feeding beneficial bacteria so they can flourish, strengthen the gut lining, and keep harmful bacteria and toxins from entering your bloodstream.
On the other hand, research shows that diets high in sugar, saturated fat, alcohol, salt, and emulsifier-rich ultra-processed foods, especially when paired with low fiber intake, are linked to a weakened gut barrier and reduced beneficial bacteria. When this occurs, local and whole-body inflammation can follow.
Simple meals, such as overnight oats, can support gut health while providing steady energy.
→ Raspberry Hemp Overnight Oats
Those with IBS or IBD may want to think twice about increasing their prebiotic/fiber intake. If you are already having severe gastric distress and symptoms, talk to your dietitian or doctor about the right amount and types of fiber for you.
Foods That May Increase Inflammation
Reduce the following foods
- Refined carbohydrates such as white bread, white pasta, French fries, and sweet baked goods.
- Foods and beverages high in added sugar or artificial additives
- Processed meats like hot dogs, bacon, and deli meats
- Fast food
- Highly processed packaged foods
Do You Need to Eliminate Gluten, Dairy, or Soy?
Some people may notice symptoms after eating certain foods like gluten, dairy, soy, or eggs. These reactions are highly individual, and eliminating foods without guidance isn’t always necessary. The goal is to discover what supports your body and what triggers discomfort so you can enjoy as much variety as possible in your diet. One of our dietitians can guide you and support you in this process.
The Big Picture
Reducing inflammation with food does not require a perfect diet. Elimination of entire food groups is not always necessary either. Instead, focus on simple habits:
- Meal plan and eat more food from home
- Include a variety of colorful plant foods in your meals and snacks
- Eat omega-3-rich fish at least twice a week
- Limit ultra-processed foods, fast foods, and excess sugary foods/drinks
Small, consistent changes can help support a healthier inflammatory response and improve long-term health.
Want Personalized Help Reducing Inflammation?
Everyone’s body responds differently to food. If you are experiencing digestive symptoms, chronic inflammation, or metabolic concerns, personalized nutrition guidance can make a big difference.
Learn more about working with a dietitian at Well Balanced Nutrition.
→ Personal Nutrition Coaching

by Kristen Norton | Mar 31, 2026 | Recipes and Meal Ideas
- 1/2 head green cabbage shredded finely
- 2 carrots grated finely
- 6 cups water
- 1 mango cut into slivers
- 3 medium 4-1/8″ long scallions, chopped
- 1/4 cup parsley
- 3 limes juiced
- 2 tablespoons olive oil
- 1 tablespoon honey
- salt to taste
Prep
Prep ingredients according to instructions.
Make
Add cabbage and carrots to a colander. Pour boiling water over vegetables and let them drain.
Add cabbage, carrots, mango, scallions, and parsley to a large bowl and toss to combine.
Whisk together lime juice, olive oil, and honey. Salt to taste.
Massage vegetables with dressing until coated.
Serve or store in refrigerator for up to 4 days.
Nutrition Facts: Calories Total Fat 7g Saturated Fat 1g Sodium 46mg Total Carbohydrates 34g Dietary Fiber 7g
Total Sugars 22g Protein 4g Calcium 133mg Iron 1mg Potassium 610mg

by Kristen Norton | Mar 24, 2026 | Recipes and Meal Ideas
Quick Strawberry Jam
- 3 cups strawberries fresh, chopped (or frozen)
- 2 Tbs. maple syrup
- 4 Tbs chia seeds
Chia Pudding
- 1 3/4 cups coconut milk unsweetened (or other milk)
- 1/2 cup chia seeds
- 2 tsp. vanilla extract
- 2 Tbs maple syrup
Prep Jam
Hull and chop strawberries
Make Jam
Add strawberries and maple syrup to a small saucepan.
Simmer until the fruit breaks down, then bring to a boil and simmer for an additional 10-15 minutes until fruit is soft and the mixture is thickened.
Stir in chia seeds and set aside to cool.
Make Pudding
Add all ingredients to a mason jar fitted with a lid and shake to combine. Set aside for 10 minutes.
Shake or stir again. In separate serving. jars, layer chia pudding with cooled strawberry jam and place in the refrigerator for 4 hours or overnight.
Nutrition Facts: Calories 322 Total Fat 16g Saturated Fat 1g Sodium 125mg Total Carbohydrates 37g
Dietary Fiber 14gT otal Sugars 19g Protein 10g Calcium 507mg Iron 5mg Potassium 423mg